3D-printing non-toxic biocompatible medical implants
October 25, 2013
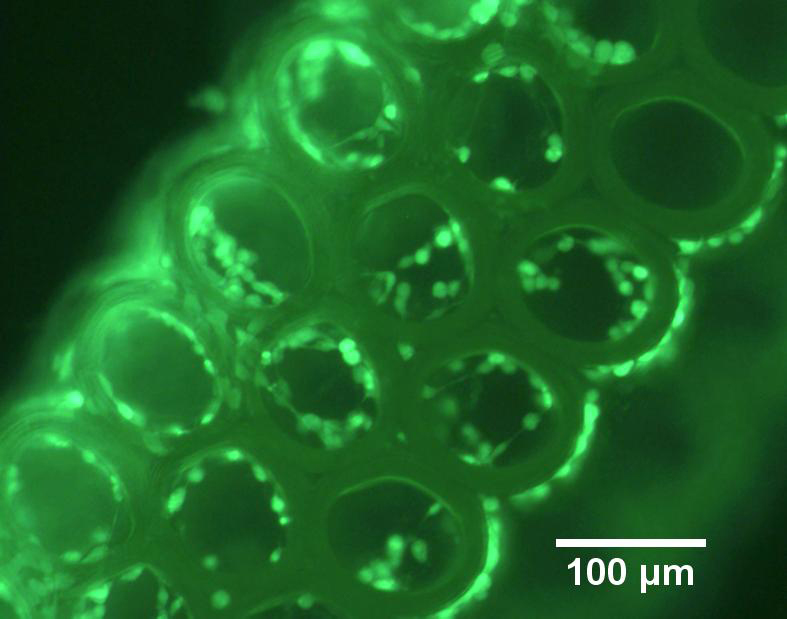
A common vitamin now allows researchers to create finely-detailed, biocompatible structures, such as this scaffold for tissue engineering (credit: Regenerative Medicine)
A common vitamin — riboflavin (vitamin B2) — has made it possible to 3D-print non-toxic medical implants, researchers from North Carolina State University, the University of North Carolina at Chapel Hill and Laser Zentrum Hannover have discovered.
“This opens the door to a much wider range of biocompatible implant materials, which can be used to develop customized implant designs using 3-D printing technology,” says Dr. Roger Narayan, senior author of a paper describing the work and a professor in the joint biomedical engineering department at NC State and UNC-Chapel Hill.
Using light to create create implants
The researchers in this study focused on a 3-D printing technique called two-photon polymerization, because this technique can be used to create small objects with detailed features — such as scaffolds for tissue engineering, microneedles, or other implantable drug-delivery devices.
Two-photon polymerization is a 3-D printing technique for making small-scale solid structures from many types of photoreactive liquid precursors. The liquid precursors contain chemicals that react to light, turning the liquid into a solid polymer. By exposing the liquid precursor to targeted amounts of light, the technique allows users to “print” 3-D objects.
Two-photon polymerization has its drawbacks, however. Most chemicals mixed into the precursors to make them photoreactive are also toxic, which could be problematic if the structures are used in a medical implant or are in direct contact with the body.
But the researchers have found that riboflavin — is both nontoxic and biocompatible — can become photoreactive be mixed with a precursor material such as triethanolamine.
No, you can’t make your own DIY implants on your home or office 3D printer (yet).
The research was supported by a National Science Foundation grant.
Abstract of Regenerative Medicine paper
Aim: In this study, the suitability of a mixture containing riboflavin (vitamin B2) and triethanolamine (TEOHA) as a novel biocompatible photoinitiator for two-photon polymerization (2PP) processing was investigated. Materials & methods: Polyethylene glycol diacrylate was crosslinked using Irgacure® 369, Irgacure 2959 or a riboflavin–TEOHA mixture; biocompatibility of the photopolymer extract solutions was subsequently assessed via endothelial cell proliferation assay, endothelial cell viability assay and single-cell gel electrophoresis (comet) assay. Use of a riboflavin–TEOHA mixture as a photoinitiator for 2PP processing of a tissue engineering scaffold and subsequent seeding of this scaffold with GM-7373 bovine aortic endothelial cells was also demonstrated. Results: The riboflavin–TEOHA mixture was found to produce much more biocompatible scaffolds than those produced with Irgacure 369 or Irgacure 2959. Conclusion: The results suggest that riboflavin is a promising component of photoinitiators for 2PP fabrication of tissue engineering scaffolds and other medically relevant structures (e.g., biomicroelectromechanical systems).
Dr. Roger Narayan:
1. What are the practical uses of this innovation?
Polyethylene glycol diacrylate (PEGda) hydrogels can be used as materials for some biomedical applications since their mechanical properties can be altered by modifying the concentration and/or molecular weight [1]. Bulick et al. and Munoz-Pinto et al. have stated that PEGda is commonly utilized as a “model” scaffold material for growth of fibroblast-like cells or smooth muscle–like cells [2, 3]. Bulick et al. developed PEGda scaffolds for tissue engineering including smooth muscle cells, in which the crosslinking of PEGda and the slow degradation rate of PEGda enabled immobilization of cells within the scaffold [2]. PEGda hydrogels may be useful for cartilage tissue engineering since cells are embedded by the crosslinked material; chondrocyte photoencapsulation has been examined using in vitro and in vivo studies [4]. Use of PEGda scaffolds for encapsulation of human mesenchymal stem cells has also been shown [5]. In addition to use as a material for tissue engineering applications, PEGda hydrogel structures may have other in vivo applications. For example, PEGda may be used in wound dressings and vascular graft coatings [6]. PEGda can also be used as a filler material for soft tissue restoration since it is low in cost, nonpyrogenic, and nonallergenic [7]. Patel et al. showed that PEGda is able to withstand forces that are associated with soft tissue filler applications [8].
[1] Liao H, Munoz-Pinto D, Qu X, Hou Y, Grunlan MA, and Hahn MS. Influence of hydrogel mechanical properties and mesh size on vocal fold fibroblast extracellular matrix production and phenotype. Acta Biomater. 4(5), 1161-71 (2008).
[2] Bulick AS, Muñoz-Pinto DJ, Qu X, Mani M, Cristancho D, Urban M, and Hahn MS. Impact of endothelial cells and mechanical conditioning on smooth muscle cell extracellular matrix production and differentiation. Tissue Eng. Part A 15(4), 815-25 (2009).
[3] Munoz-Pinto DJ, Bulick AS, and Hahn MS. Uncoupled investigation of scaffold modulus and mesh size on smooth muscle cell behavior. J. Biomed. Mater. Res. A 90(1), 303-16 (2009).
[4] Lin S, Sangaj N, Razafiarison T, Zhang C, and Varghese S. Influence of physical properties of biomaterials on cellular behavior. Pharm Res. 28(6), 1422-30 (2011).
[5] Bahney CS, Lujan TJ, Hsu CW, Bottlang M, West JL, and Johnstone B. Visible light photoinitiation of mesenchymal stem cell-laden bioresponsive hydrogels. Eur. Cell Mater. 22, 43-55 (2011).
[6] Browning MB, Cosgriff-Hernandez E. Development of a Biostable Replacement for PEGDA Hydrogels. Biomacromolecules 13, 779-786 (2012)
[7] Xin AX, Gaydos C, Mao JJ. In vitro degradation behavior of photopolymerized PEG hydrogels as tissue engineering scaffold. Presented at: EMBS Annual International Conference. New York City, USA. Aug 30-Sept 3 (2006)
[8] Patel PN, Smith CK, and Patrick CW Jr. Rheological and recovery properties of poly(ethylene glycol) diacrylate hydrogels and human adipose tissue. J. Biomed. Mater. Res. A. 73(3), 313-9 (2005).
2. When can we expect this innovation to be available commercially?
Several 3D printed devices are currently available, such as Invisalign braces. 3D printed parts using a more biocompatible riboflavin-based photoinitiator can be readily translated to use in medical device manufacturing.
3. How does this innovation compare to others?
Other groups have considered use of riboflavin and other biocompatible photoinitiators for use with other 3D printing technologies. This paper is the first that shows use of a riboflavin-based photoinitiator with two-photon polymerization, a 3D printing technique that creates much smaller structures than other 3D printing techniques.