A fiber-optic method of arresting epileptic seizures
February 5, 2013
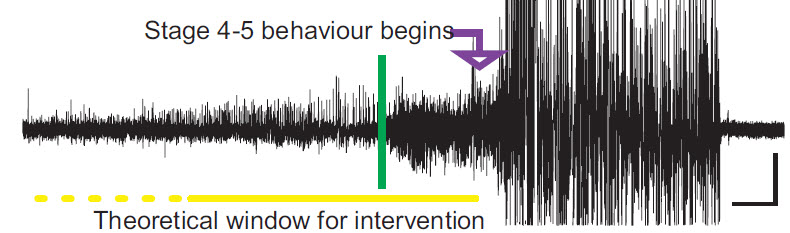
Blocking a seizure. The vertical green bar indicates online seizure detection, prior to the start of stage 4–5 behavior (arrow). The yellow bars under the trace highlight the theoretical window for intervention.
UC Irvine neuroscientists have developed a way to stop epileptic seizures with fiber-optic light signals, heralding a novel opportunity to treat the most severe manifestations of the brain disorder.
Using a mouse model of temporal lobe epilepsy, Ivan Soltesz, Chancellor’s Professor and chair of anatomy & neurobiology, and colleagues created an EEG-based brain-waves-sensing) computer system that lights up hair-thin fiber optic strands implanted in the brain when it detects a real-time seizure.
These fibers “turn on” specially expressed, light-sensitive proteins called opsins, which can either stimulate or inhibit specific neurons in select brain regions during seizures, depending on the type of opsin.
The researchers found that this process was able to arrest ongoing electrical seizure activity and reduce the incidence of severe “tonic-clonic” events.
“This approach is useful for understanding how seizures occur and how they can be stopped experimentally,” Soltesz said. “In addition, clinical efforts that affect a minimum number of cells and only at the time of a seizure may someday overcome many of the side effects and limitations of currently available treatment options.”
More than 3 million Americans suffer from epilepsy, a condition of recurrent spontaneous seizures that occur unpredictably, often cause changes in consciousness, and can preclude normal activities such as driving and working. In at least 40 percent of patients, seizures cannot be controlled with existing drugs, and even in those whose seizures are well controlled, the treatments can have major cognitive side effects.
Although the study was carried out in mice, not humans, Soltesz said the work could lead to a better alternative to the currently available electrical stimulation devices.
The study was supported by the National Institutes of Health, the Epilepsy Foundation, and the George E. Hewitt Foundation for Medical Research.