A microchip for studying cancer metastasis
February 7, 2014
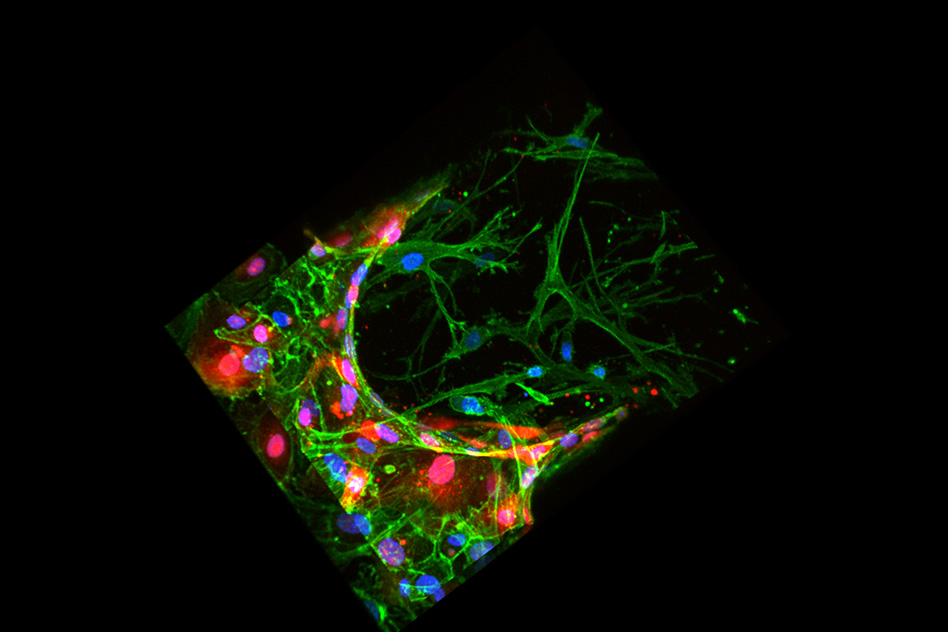
A three-dimensional reconstruction of a confocal image of a bone-mimicking microenvironment (green). Endothelial cells (red) mimic blood vessels; breast cancer cells (blue) are passing through the endothelial wall, into the bone-like matrix. (Credit: Jessie Jeon)
To visualize how cancer cells invade specific organs, researchers from MIT, Italy, and South Korea have developed a three-dimensional microfluidic platform (microchip) that mimics the spread of breast cancer cells into a bonelike environment.
(Nearly 70 percent of patients with advanced breast cancer experience skeletal metastasis, in which cancer cells migrate from a primary tumor into bone — a painful development that can cause fractures and spinal compression. Not much is known about how and why certain cancers spread to specific organs, such as bone, liver, and lungs.)
The microchip contains several channels in which the researchers grew endothelial cells (that line the interior surface of blood vessels) and bone cells to mimic a blood vessel and bone side-by-side. They then injected a highly metastatic (tend to spread in the body) line of breast cancer cells into the fabricated blood vessel.
Rapid spread of cancer cells into bone
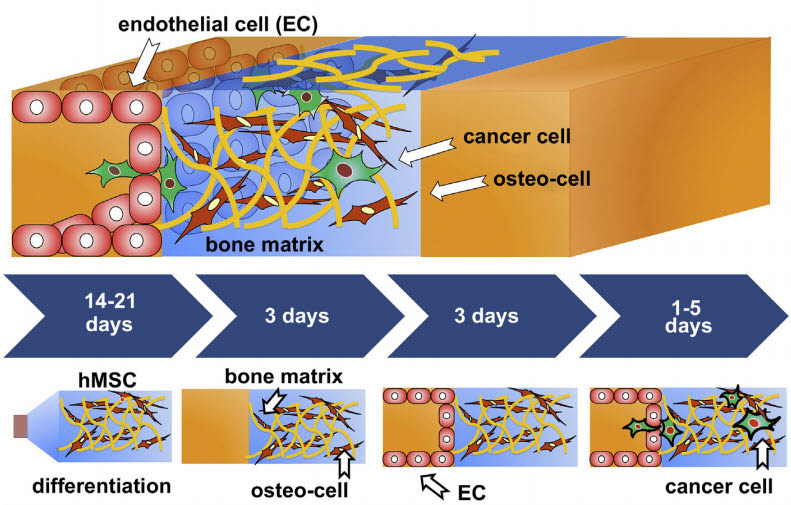
Cancer cells quickly metastsize (spread) through the blood vessel wall and into the bonelike environment (credit: Simone Bersini et al./Biomaterials)
Twenty-four hours later, the team observed that twice as many cancer cells had made their way through the vessel wall and into the bonelike environment than had migrated into a simple collagen-gel matrix. Moreover, the cells that made it through the vessel lining and into the bonelike setting formed microclusters of up to 60 cancer cells by the experiment’s fifth day.
“You can see how rapidly they are growing,” says Jessie Jeon, a graduate student in mechanical engineering. “We only waited until day five, but if we had gone longer, [the size of the clusters] would have been overwhelming.”
The team also identified two molecules that appear to encourage cancer cells to metastasize: CXCL5, a protein ligand secreted by bone cells, and CXCR2, a receptor protein on cancer cells that binds to the ligand. The preliminary results suggest that these molecules may be potential targets to reduce the spread of cancer.
Jeon says the experiments demonstrate that the microchip may be used in the future to test drugs that might block metastasis, and also as a platform for studying cancer’s spread to other organs.
She and her colleagues, including Roger Kamm, the Cecil and Ida Green Distinguished Professor of Mechanical and Biological Engineering at MIT, have outlined the results of their experiments in the journal Biomaterials.
“Currently, we don’t understand why certain cancers preferentially metastasize to specific organs,” Kamm says. “An example is that breast cancer will form metastatic tumors in bone, but not, for example, muscle. Why is this, and what factors determine it? We can use our model system both to understand this selectivity, and also to screen for drugs that might prevent it.”
The next stage of metastasis
Now the group is looking to the next step in metastasis: the stage at which a cancer cell invades a specific organ. In particular, the researchers designed a microchip in which they could observe interactions between specific cancer cells and a receptive, organlike environment.
Jeon and her colleagues captured images of the metastatic process: Cancer cells pushed through the vessel wall, spread into the bonelike environment, and clustered deep in the bone matrix to form tiny tumors. They found that twice as many cancer cells spread to the bonelike environment compared to a standard collagen matrix; these also spread deeper into the bone matrix, forming microclusters of up to 60 cells after five days.
To see what molecular signals might explain the difference in metastatic rate, the team focused on CXCL5 and CXCR2. While these two proteins are known to have a role in metastasis, it’s not clear whether they promote it in specific organs.
The researchers incubated cancer cells with an antibody that blocked CXCR2, and found that these cells were less able to break through the blood vessel lining. They also tried injecting CXCL5 into a collagen-gel matrix without bone cells, and found that the ligand-seeded environment encouraged breast cancer cells to invade. The results suggest these two proteins may be targets for preventing or mitigating cancer metastasis not just in bone, but in other organs as well.
The team plans to explore cancer metastasis in other organs, such as muscle — an organ in which cancer cells do not easily spread.
In the future, such a platform may be used in personalized medicine to determine the best cancer therapy for a given patient. “One might envision using cells from the cancer patient to produce models of different organs, then using these models to determine the optimal therapy from a variety of available drugs,” Kamm says.
This research was supported by the National Cancer Institute and the Italian Ministry of Health.
Abstract of Biomaterials paper
Cancer metastases arise following extravasation of circulating tumor cells with certain tumors exhibiting high organ specificity. Here, we developed a 3D microfluidic model to analyze the specificity of human breast cancer metastases to bone, recreating a vascularized osteo-cell conditioned microenvironment with human osteo-differentiated bone marrow-derived mesenchymal stem cells and endothelial cells. The tri-culture system allowed us to study the transendothelial migration of highly metastatic breast cancer cells and to monitor their behavior within the bone-like matrix. Extravasation, quantified 24 h after cancer cell injection, was significantly higher in the osteo-cell conditioned microenvironment compared to collagen gel-only matrices (77.5 ± 3.7% vs. 37.6 ± 7.3%), and the migration distance was also significantly greater (50.8 ± 6.2 μm vs. 31.8 ± 5.0 μm). Extravasated cells proliferated to form micrometastases of various sizes containing 4 to more than 60 cells by day 5. We demonstrated that the breast cancer cell receptor CXCR2 and the bone-secreted chemokine CXCL5 play a major role in the extravasation process, influencing extravasation rate and traveled distance. Our study provides novel 3D in vitro quantitative data on extravasation and micrometastasis generation of breast cancer cells within a bone-like microenvironment and demonstrates the potential value of microfluidic systems to better understand cancer biology and screen for new therapeutics.