Alzheimer’s researchers creating ‘designer tracker’ to quantify elusive brain protein, provide earlier diagnosis
April 26, 2013
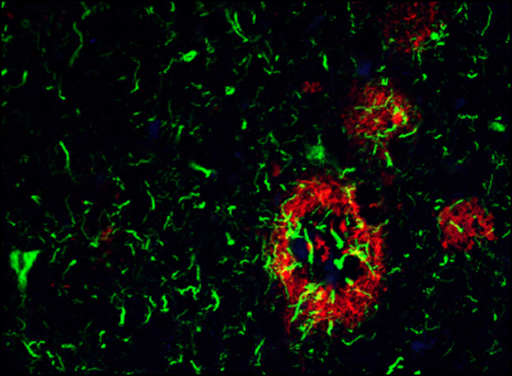
Dual channel fluoresecence microscopy of Alzheimer’s disease brain reveals presence of extracellular Abeta- (red) and intracellular tau- (green) bearing lesions (credit: Kristen E Funk, PhD)
By using computer-aided drug discovery, an Ohio State University molecular biochemist and molecular imaging chemist are collaborating to create an imaging chemical that attaches predominantly to tau-bearing lesions in living brain.
Their hope is that the “designer” tracer will open the door for earlier diagnosis — and better treatments for Alzheimer’s, frontal temporal dementia and traumatic brain injuries like those suffered by professional athletes, all conditions in which tangled tau filaments accumulate in brain tissue.
“We’re creating agents that are specifically engineered to bind the surface of aggregated tau proteins so that we can see where and how much tau is collecting in the brain,” said Jeff Kuret, professor of molecular and cellular biochemistry at The Ohio State University College of Medicine. “We think the “tau signature” can be used to improve diagnosis and staging of disease.”
One of the biggest challenges with Alzheimer’s disease (AD) is that by the time physicians can detect behavioral changes, the disease has already begun its irreversibly destructive course.
Scientists know toxic brain lesions created by amyloid beta and tau proteins are involved. Yet, emerging therapies targeting these lesions have failed in recent clinical trials. These findings suggest that successful treatments will require diagnosis of disease at its earliest stages.
Tauopathies are neurodegenerative diseases associated with the accumulation of tau protein “tangles” in the human brain. Alzheimer’s disease is one of the most common tauopathies, but tau aggregates are also found in certain forms of frontal temporal dementia as well as traumatic brain injuries. Alzheimer’s disease has become one of the most common disorders in the aging population, and is predicted to be a major driver of health care costs in the coming decades.
The study’s co-investigator, Michael Tweedle, a professor of radiology at Ohio State’s College of Medicine, notes that there may be more advantages to being able to image tau.
“Unlike beta amyloid, tau appears in specific brain regions in Alzheimer’s,” said Tweedle. “With a better view of how tau is distinct from amyloid, we’ll be able to create a much more accurate view of disease staging, and do a much better job getting the right therapeutics into the right populations at the right time.”
Tweedle notes that there are no drugs currently available that target tau, but that several are in development. Both investigators emphasized that being able to image tau in a living brain could be critical for identifying individuals that could benefit from tau-tackling drugs as they move into clinical trials.
The search for tau selective neuroimaging agents is proceeding. So far, the team has prepared 12 ligands that have promising binding affinity for tau aggregates.
“It’s an iterative process, and each step gives us new information on what we need to be looking for,” said Tweedle. “Now we know what parts of the molecule to alter while trying to retain other good qualities.”
Research funding was from a pilot grant awarded to the team by Ohio State’s Center for Clinical and Translational Science (CCTS). The award provided them with the funds needed to synthesize candidate radiotracers for testing. The team then received funding from the Alzheimer’s Drug Discovery Foundation to test how the compounds distribute throughout the body. This work also leverages several CCTS-funded core resources.