Artificial pancreas and algorithm improve treatment for type 1 diabetes
January 30, 2013
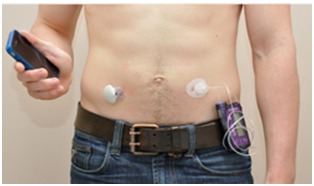
External artificial pancreas includes a continual glucose monitor (left), pump worn on the belt that injects insulin under the patient’s skin (right), and a controller (here, a handheld smartphone) (credit: Ahmad Haidar et al./Institut de recherches cliniques de Montreal)
The first trial comparing a new dual-hormone “artificial pancreas” with conventional diabetes treatment using an insulin pump has been completed by researchers at IRCM (Institut de Recherches Cliniques) of Montreal, led by endocrinologist Dr. Rémi Rabasa-Lhoret. It showed improved glucose levels and lower risks of hypoglycemia.
How it works
The artificial pancreas developed at IRCM is an automated system that simulates the normal pancreas by continuously adapting insulin delivery based on changes in glucose levels.
The dual-hormone artificial pancreas controls glucose levels by automatically delivering both insulin and glucagon hormones, when necessary, based on continuous glucose monitor (CGM) readings and guided by an advanced algorithm.
“We found that the artificial pancreas improved glucose control by 15 per cent and significantly reduced the risk of hypoglycemia as compared with conventional insulin pump therapy,” explains engineer Ahmad Haidar, first author of the study and doctoral student in Dr. Rabasa-Lhoret’s research unit at the IRCM and at the Department of Electrical and Computer Engineering at McGill University.
“The artificial pancreas also resulted in an 8-fold reduction of the overall risk of hypoglycemia, and a 20-fold reduction of the risk of nocturnal hypoglycemia.”
Background
People living with type 1 diabetes must carefully manage their blood glucose levels to ensure they remain within a target range. Blood glucose control is the key to preventing serious long-term complications related to high glucose levels (such as blindness or kidney failure) and reduces the risk of hypoglycemia (dangerously low blood glucose that can lead to confusion, disorientation and, if severe, loss of consciousness).
“Approximately two-thirds of patients don’t achieve their target range with current treatments,” says Dr. Rabasa-Lhoret, Director of the Obesity, Metabolism and Diabetes research clinic at the IRCM. “The artificial pancreas could help them reach these targets and reduce the risk of hypoglycemia, which is feared by most patients and remains the most common adverse effect of insulin therapy. In fact, nocturnal hypoglycemia is the main barrier to reaching glycemic targets.”
“Infusion pumps and glucose sensors are already commercially-available, but patients must frequently check the sensor and adjust the pump’s output,” says Haidar. “To liberate them from this sizable challenge, we needed to find a way for the sensor to talk to the pump directly.
Intelligent dosing algorithm
“So we developed an intelligent dosing algorithm, which is the brain of the system. It can constantly recalculate insulin dosing based on changing glucose levels, in a similar way to the GPS system in a car, which recalculates directions according to traffic or an itinerary change.”
The algorithm receives data from the continuous glucose monitor, calculates the required insulin (and glucagon, if needed) and wirelessly controls the pump to automatically administer the proper doses without intervention by the patient. The algorithm could eventually be integrated as software into a smartphone,
“The system we tested more closely mimics a normal pancreas by secreting both insulin and glucagon,” adds Dr. Laurent Legault, peadiatric endocrinologist and outgoing Director of the Insulin Pump Centre at the Montreal Children’s Hospital, and co-author of the study. “While insulin lowers blood glucose levels, glucagon has the opposite effect and raises glucose levels. Glucagon can protect against hypoglycemia if a patient with diabetes miscalculates the necessary insulin dose.”
“Our work is exciting because the artificial pancreas has the potential to substantially improve the management of diabetes and reduce daily frustrations for patients,” concludes Rabasa-Lhoret. “We are pursuing our clinical trials to test the system for longer periods and with different age groups. It will then probably be introduced gradually to clinical practice, using insulin alone, with early generations focusing on overnight glucose controls.”
The study was conducted with 15 adult patients with type 1 diabetes, who had been using an insulin pump for at least three months. Patients were admitted twice to the IRCM’s clinical research facility and received, in random order, both treatments: the dual-hormone artificial pancreas and the conventional insulin pump therapy. During each 15-hour visit, their blood glucose levels were monitored as they exercised on a stationary bike, received an evening meal and a bedtime snack, and slept at the facility overnight.
Dr. Rabasa-Lhoret’s research is funded by Diabetes Québec, the Canadian Diabetes Association, and the IRCM’s J.A. De Sève Chair in clinical research. IRCM collaborators who contributed to study include Maryse Dallaire, Ammar Alkhateeb, Adèle Coriati, Virginie Messier and Maude Millette.