Every breath you take, every move you make …
September 19, 2011 by Amara D. Angelica
Breath detector (credit: University of Utah)
Those University of Utah engineers who built wireless networks that see through walls are now taking it a step further: detecting if surgery patients, adults with sleep apnea, and babies at risk of sudden infant death syndrome (SIDS) have stopped breathing.
This thing freaks me out a bit. Think what Homeland Security could do with it. The idea of being surrounded by tiny microwave ovens would be enough to make me stop breathing.
They plan to use low-cost wireless wireless transceivers similar to those used in home computer networks, making their “BreathTaking” system cheaper than existing methods of monitoring breathing, says Neal Patwari, UU assistant professor of electrical engineering.
The American Academy of Pediatrics says there is “no evidence that home monitors are effective” for preventing SIDS. Since 2005, the group has opposed the use of breathing monitors to prevent SIDS, but has said they “may be useful in some infants who have had an apparent life-threatening event,” including some combination of apnea [abnormal interruptions in breathing], color change, limpness and choking or gagging.
“The AAP recognizes that monitors may be helpful to allow rapid recognition of apnea, airway obstruction, respiratory failure, interruption of supplemental oxygen supply, or failure of mechanical respiratory support,” the group states.
SIDS monitors now on the market include FDA-approved medical devices that measure heart rate and respiration and are connected to babies with wires, electrodes and-or belts. Other monitors, which are non-medical and over-the-counter versions, detect a lack of sound, or use mattress sensors to detect a lack of movement.
Patwari says that with the new method, “the patient or the baby doesn’t have to be connected to tubes or wired to other sensors, so they can be more comfortable while sleeping. If you’re wired up, you’re going to have more trouble sleeping, which is going to make your recovery in the hospital worse.”
Some opposition to SIDS monitors is based on a fear that parents will depend on monitors instead of following other, more effective medical measures, including always placing babies on their backs to sleep, keeping redundant bedding and soft objects out of the crib, and not having babies share a bed with adults.
The researcher formed a University of Utah spinoff company, Xandem Technology LLC, which is commercializing the wireless networks for use as motion detectors for burglar alarm systems, to help police locate hostages and even to alert out-of-town, vacationing parents if a crowd of teenagers is partying at their home during their absence.
“A search and rescue team may arrive at a collapsed building and throw transceivers into the rubble, hoping to detect the breathing of anyone still alive inside,” Patwari and colleagues write. “Police or SWAT teams may deploy a network around a building to determine if people are inside.”
Privacy worries
“On the other hand, the ability to measure breathing from a wireless network has privacy implications,” they add. “We have shown previously that a network deployed around external walls of a building can detect and track a person who is moving or changing position. If this system can also detect and monitor a sleeping person’s breathing, it would have additional utility for eavesdroppers or thieves.”
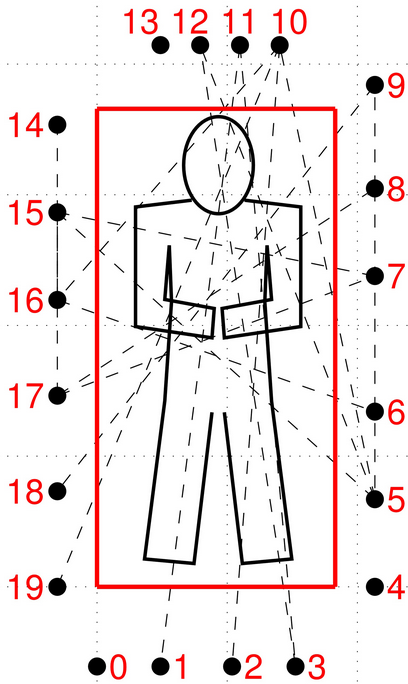
The motion of the chest and abdomen during breathing impedes the wireless radio signals crisscrossing a bedridden patient, who in the study was Patwari himself. Each of the 20 transceivers or “nodes” can transmit and receive to the other 19, meaning there can be up to 380 measurements (20 times 19) of radio signal strength within a short period of time (the transceivers transmit one after the other).
The study found the wireless network could measure breathing within 0.4 to 0.2 breaths per minute, an insignificant error rate given that most breathing monitors round to the nearest breath per minute, he says. If a bedridden person or baby moves, the wireless system detects the movement but cannot measure their breathing at the same time.
Patwari also measured how many nodes were required to measure breathing accurately. The minimum was 13 nodes or transceivers, while the rate of incorrect breathing measurements fell to zero when 19 nodes were used. The study also showed the height of the nodes around the hospital bed didn’t significantly affect breathing measurements.
He also wants to test whether the system can detect two people breathing at the same rate but not in sync — something that might make it possible to design a system that could detect not only the location of hostages in a building, but the number held together.
Ref.: Neal Patwari et al., ArXiv, 2011; [in press]