Guinea pig hearts beat with human cells
August 6, 2012
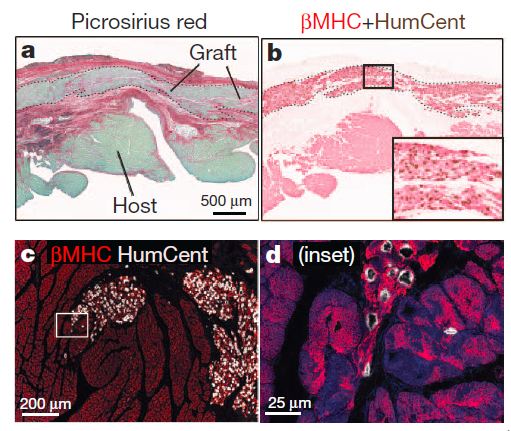
Transplanted hESC-CMs partially remuscularize injured guinea-pig hearts, preserve mechanical function and reduce arrhythmia susceptibility. a, b, Twenty-eight-day-old hESC-CM grafts in a cryoinjured heart stained with picrosirius red (a), and anti-b-myosin heavy chain (bMHC, red) plus human-specific in situ probe (HumCent, brown) (b). c–d, Confocal image of host–graft contact, dual-labelled for HumCent (white) and bMHC (red) (c; a higher magnification image of the area in the white box in c is shown in d). (Credit: Yuji Shiba et al./Nature)
University of Washington research raises hopes for cell therapies, showing that heart muscle cells differentiated from human embryonic stem cells can integrate into existing heart muscle, Nature News reports.
“What we have done is prove that these cells do what working heart muscles do, which is beat in sync with the rest of the heart,” says Chuck Murry, a cardiovascular biologist at the University of Washington in Seattle, who co-led the research.
Cardiomyocytes derived from human embryonic stem (ES) cells typically beat fewer than 150 times a minute. External electrical stimulation can increase that rate, but only up to about 240 beats per minute, says Michael LaFlamme, a cardiovascular biologist at the University of Washington and the other co-leader on the project. Rats and mice have heart rates of around 400 and 600 beats per minute, respectively.
However, guinea pigs have a heart rate of 200–250 beats per minute, near the limit for human cardiomyocytes. From the first experiment with the sensor in guinea pigs, it was obvious that the transplanted cells were beating in time with the rest of the heart, says LaFlamme. When he looked into the chest cavity, the heart “was flashing back at us”, he says.
Both Murry and LaFlamme agree that much more work needs to be done before transplantable cardiomyocytes are ready for human trials. The more immediate goal, says LaFlamme, is to hunt for experimental conditions that allow cells to engraft in scar tissue more thoroughly.