Handheld 3D medical scanner to provide high-resolution 3D imaging in doctor’s offices
October 4, 2012

Handheld scanner with interchangeable tips for imaging various tissue sites (credit: Stephen A. Boppart)
University of Illinois at Urbana-Champaign (UIUC) engineers have created a handheld scanner to enable primary care physicians to image conmon sites, such as bacterial colonies in the middle ear or the thickness and health of patients’ retinas.
In the operating room, surgeons can see inside the human body in real time using advanced imaging techniques, but primary care physicians haven’t commonly had access to the same technology — until now.
To monitor chronic conditions, primary care physicians currently rely on instruments that are essentially magnifying glasses, says UIUC physician and biomedical engineer Stephen Boppart, who will present the team’s findings at the Frontiers in Optics conference* on Oct. 16.
The new handheld imaging device would give doctors a way to quantitatively monitor these conditions, and possibly make more efficient and accurate referrals to specialists.
The device relies on optical coherence tomography (OCT), a visualization technology similar to ultrasound imaging. It generates high-resolution, real-time, 3D images of the multiple tissue sites commonly examined during primary care outpatient exams, including the eyes, ears, oral and nasal mucosa, skin, and cervix
Two examples
According to Boppart, “recent evidence has strongly associated chronic, recurrent episodes of otitis media with the presence of middle ear bacterial biofilms, and currently no non-invasive means exists to detect and quantify, let alone longitudinally monitor, these structures, which act as reservoirs for antibiotic-resistant bacteria for seeding recurrent infections.
“The rapidly rising prevalence of obesity has already been followed by increases in diabetes among increasingly younger patients, along with the associated complications of this disease, such as diabetic retinopathy. The successful use of OCT in ophthalmology can subsequently be advanced to the front-line of primary care to monitor patients for early evidence of diabetic retinopathy, and to quantify longitudinal changes during treatment.”
How it works
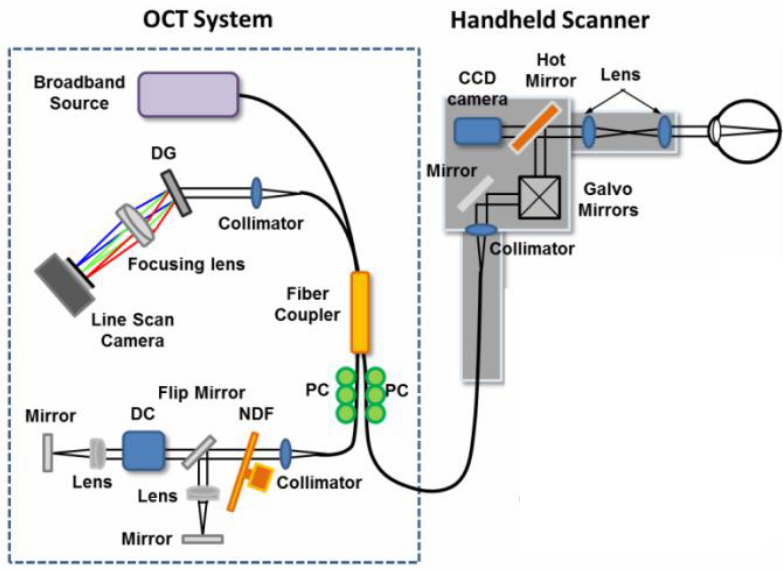
The OCT-based scanner includes three basic components: a near-infrared light source (“Broadband Source”) to generate near-infrared light (sent to the scanner via fiber cable), a video camera (“CCD camera”) to relay real-time images of surface features and scan locations, and a microelectromechanical (MEMS)-based scanner (right) to direct the light. The handheld scanner and system can simultaneously generate and display images from both the CCD video camera (tissue surface) and the high-resolution OCT line-scan camera (depth-resolved tissue structures). (Credit: Stephen A. Boppart)
Near-infrared wavelengths of light penetrate deeper into human tissues than other wavelengths more readily absorbed by the body. By measuring the time it takes the light to bounce back from tissue microstructure, computer algorithms build a picture of the structure of tissue under examination.
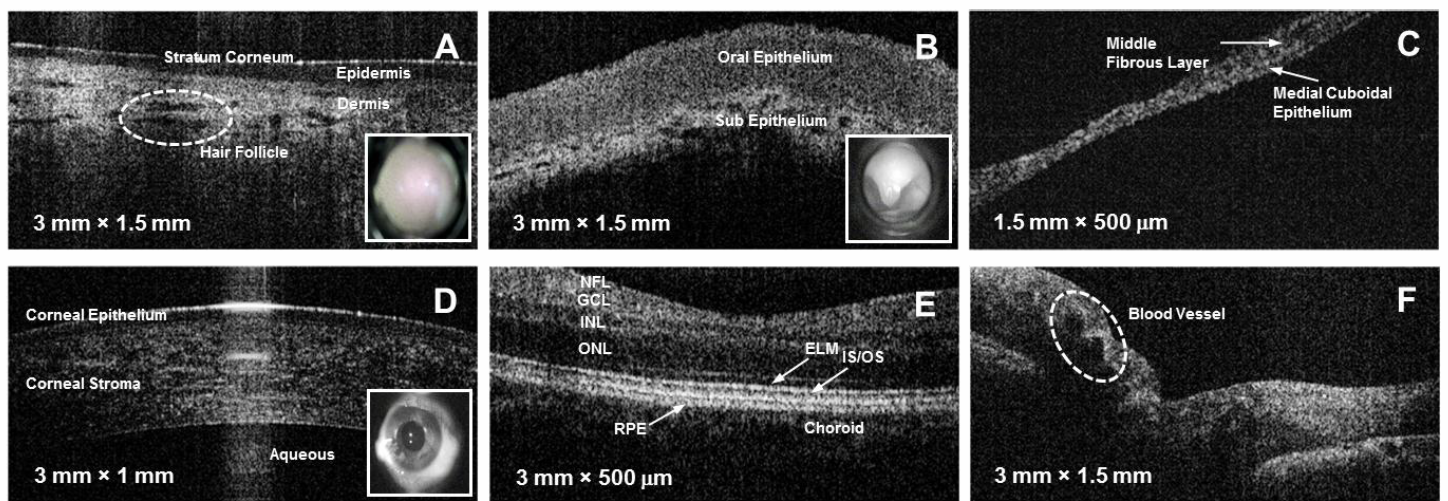
Representative high-resolution OCT images of various tissue sites of interest in primary care medicine. All images were collected in vivo from human volunteers or patients. (A) Forearm skin, (B) oral mucosa, (C) tympanic membrane, (D) cornea, (E) foveal region of retina, (F) optic disc. (Credit: Stephen A. Boppart)
Diabetic patients in particular may benefit from the device. About 40 to 45 percent of diabetics develop leaky blood vessels in their retinas — a condition called retinopathy, which can lead to thickening of the retina, blurry vision, and eventually blindness. The handheld OCT device would allow doctors to monitor the health of the retina, potentially catching retinopathy in its early stages. In some cases, changes in the eye could help doctors diagnose diabetes, Boppart says.
Boppart and his team are hopeful that falling production costs combined with smaller, more compact designs will enable more physicians to take advantage of the scanners, and become a common point-of-care tool. Eventually, they would like to see the imagers at work in developing countries as well.
He and an international team of collaborators recently received a $5 million National Institutes of Health Bioengineering Research Partnership grant to further refine the device.
* Presentation FTu2C.3. “Primary Care Imaging using Optical Coherence Tomography for Advanced Point-of-Care Diagnostics” at Frontiers in Optics (FiO) 2012 in Rochester, NY, Tuesday, Oct. 16.