Optogenetics for treating obsessive-compulsive disorders
June 18, 2013
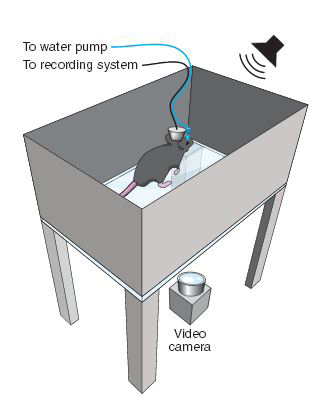
Obsessive-compulsive mice exhibit a defective grooming response during a conditioning task (credit: Eric Burguière et al./Science)
By applying optogenetics (light stimulation) to specific neurons in the brain, researchers at INSERM (Institut national de la santé et de la recherche médicale) have re-established normal behavior in mice with pathological repetitive behavior similar to that observed in human patients suffering from obsessive-compulsive disorders.
Repetitive obsessive-compulsive disorders can become a real handicap to daily life (for example, washing hands up to 30 times a day; or checking excessively that a door is locked, etc.). Obsessive-compulsive disorders affect 2 to 3% of the population and in France, it is estimated that over one million persons are affected by this disorder.
The usual treatment for obsessive-compulsive disorders is to use pharmacological treatments (anti-depressants, neuroleptics) and/or behavioral psychotherapy. They don’t work in around one third of patients.
So it is necessary to gain better understanding of the cerebral mechanisms that cause these repetitive behavior patterns in order to provide better treatment.
Previous neuroimaging studies allowed the INSERM scientists to identify dysfunctional neuron circuits located between the front of the brain (the orbitofrontal cortex) and more deep-seated cerebral structures (ganglions at the base on the brain), in certain persons suffering from obsessive-compulsive disorders.
In this new study, Eric Burguière and his co-workers (in the laboratory of Prof. Ann Graybiel in MIT) concentrated their research on this neuron circuit to examine its function in detail and also to develop an approach to treating obsessive-compulsive disorders in a mutant mouse model.
In these mutant mice, the obsessive behavior was expressed by repeated grooming all day long, to such an extent that it caused cutaneous lesions. From a physiological point of view, these animals are failing to express a protein (caused by the absence of a gene Sapap3) that is normally present in the stratial neuron synapses, a structure that is part of the ganglions at the base of the brain and is involved in functions such as learning sequences, developing habits, or decision-making.
Initial observations of the mice allowed the researchers to show that the emergence of compulsive behavior in mutant mice was caused by a deficiency in behavioral inhibition. The mice are unable to stop the act of grooming, even when it is no longer necessary. The researchers then used recordings of the neuron activity to show that the dysfunction of communication in the brain between the neocortex and the striatum leads to hyperactivity of stratial neurons in mice.
Using light
To check this hypothesis, they used optogenetics. This method consists in modifying the previously identified neurons to make them express light-sensitive proteins known as opsins. Since these neuron cells are more sensitive to light, it becomes possible to control their activity by exciting them or inhibiting them using a simple light beam.
When the researchers used light stimulation to excite the neurons in the cortex that send messages to the striatum, the compulsive disorders of the mice were greatly attenuated.
“Our discoveries show that selective stimulation of the circuit can re-establish normal behavior in mice that originally presented pathological repetitive behavior, similar to the type of behavior observed in certain patients suffering from obsessive-compulsive disorders.” said Burguière.
Using optogenetics may allow for identifying the role played by neuron circuits in the brain that, if found to be dysfunctional, may cause pathological behavior.
“I have indeed decided to return to France as part of an Inserm team so that I can run a parallel study on the physiological and behavioral effects of deep cerebral stimulation on patients suffering from obsessive-compulsive disorders, and on mice using the optogenetics technique, in order to get a better understanding of how light stimulation works,” said Burguière.