Scientists make human blood from human skin
November 8, 2010
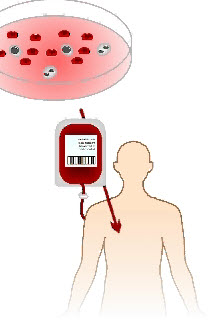 In a major breakthrough, scientists at McMaster University in Canada have discovered how to make human blood from adult human skin.
In a major breakthrough, scientists at McMaster University in Canada have discovered how to make human blood from adult human skin.
The discovery, published Sunday in Nature, could mean that in the foreseeable future, people needing blood for surgery, cancer treatment or treatment of other blood conditions like anemia will be able to have blood directly created from a patch of their own skin to provide transfusions. Clinical trials could begin as soon as 2012.
Making blood from skin does not require the middle step of changing a skin stem cell into a pluripotent stem cell that could make many other types of human cells, then turning it into a blood stem cell. It eliminates several problems with embryonic stem cells, including ethical objections, immune rejection, limited hospital resources, and limited quantities.
“We have shown this works using human skin. We know how it works and believe we can even improve on the process,” said Mick Bhatia, scientific director of McMaster’s Stem Cell and Cancer Research Institute in the Michael G. DeGroote School of Medicine. They plan to develop other types of human cell types from skin.
The discovery was replicated several times over two years using human skin from both young and old people to prove it works for any age of person.
John Kelton, hematologist and dean and vice-president of health sciences for McMaster University said: “I find this discovery personally gratifying for professional reasons. During my 30 years as a practicing blood specialist, my colleagues and I have been pleased to help care for cancer patients whose lives were saved by bone marrow transplants. For all physicians, but especially for the patients and their families, the illness became more frustrating when we were prevented from giving a bone marrow transplant because we could not find a perfect donor match in the family or the community. Dr. Bhatia’s discovery could permit us to help this important group of patients.”
“The pioneering findings published today are the first to demonstrate that human skin cells can be directly converted into blood cells, via a programming process that bypasses the pluripotent stage,” said Cynthia Dunbar, MD, Head, Molecular Hematopoiesis Section, Hematology Branch, National Heart, Lung and Blood Institute, U.S. National Institutes of Health. “Producing blood from a patient’s own skin cells, has the potential of making bone marrow transplant HLA matching and paucity of donors a thing of the past.
“Bhatia’s approach detours around the pluripotent stem cell stage and thus avoids many safety issues, increases efficiency, and also has the major benefit of producing adult-type l blood cells instead of fetal blood cells, a major advantage compared to the thus far disappointing attempts to produce blood cells from human ESCs or IPSCs.”
This research was funded by the Canadian Institutes of Health Research, the Canadian Cancer Society Research Institute, the Stem Cell Network and the Ontario Ministry of Research and Innovation.
Adapted from materials provided by McMaster University