New device yields close-up look at cancer metastasis
October 31, 2014

This dish houses a lab chip that Johns Hopkins engineers built to gain an unprecedented close-up view of how cancer cells enter the bloodstream to spread the disease. (Credit: Will Kirk/Johns Hopkins University)
Engineers at Johns Hopkins Institute for NanoBioTechnology (INBT) have invented a lab device to give cancer researchers an unprecedented microscopic look at metastasis (spread of tumor cells, causing more than 90 percent of cancer-related deaths), with the goal of eventually stopping the spread, described in their paper in the journal Cancer Report.
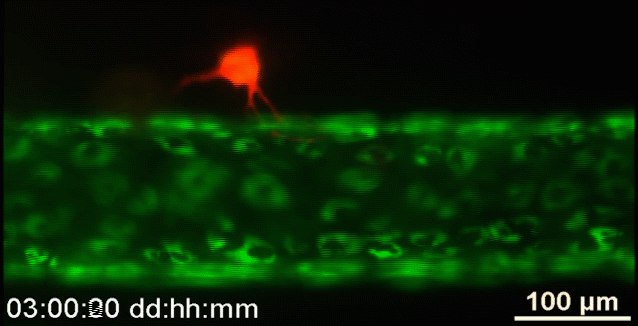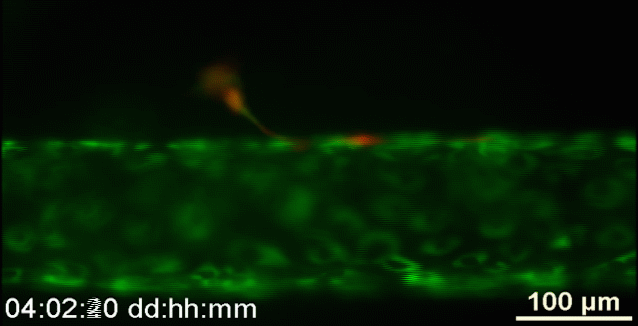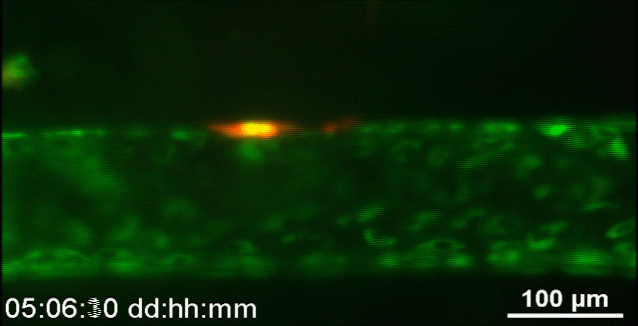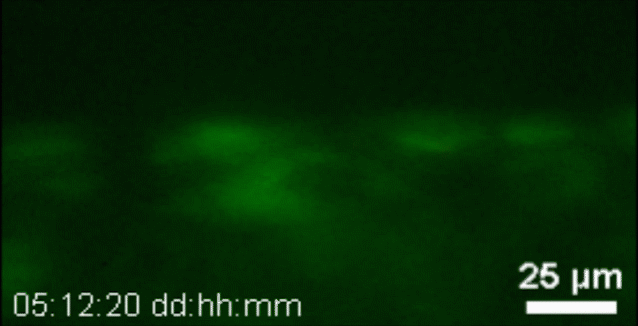
Johns Hopkins | Researchers captured this video of human breast cancer cells (red) as they burrowed through reconstituted body tissue material and made their way into an artificial blood vessel (this is an animated GIF created from the original video)
“There’s still so much we don’t know about exactly how tumor cells migrate through the body, partly because, even using our best imaging technology, we haven’t been able to see precisely how these individual cells move into blood vessels,” said Andrew D. Wong, a Department of Materials Science and Engineering doctoral student and lead author of the journal article. “Our new tool gives us a clearer, close-up look at this process.”
The device replicated these processes in a small transparent chip that incorporates an artificial blood vessel and surrounding tissue material. A nutrient-rich solution flows through the artificial vessel, mimicking the properties of blood.
With this novel lab platform, Wong said, the team was able to record a video of the movement of individual cancer cells as they crawled through a three-dimensional collagen matrix. This material resembles the human tissue that surrounds tumors when cancer cells break away and try to relocate elsewhere in the body. This process is called “invasion.”
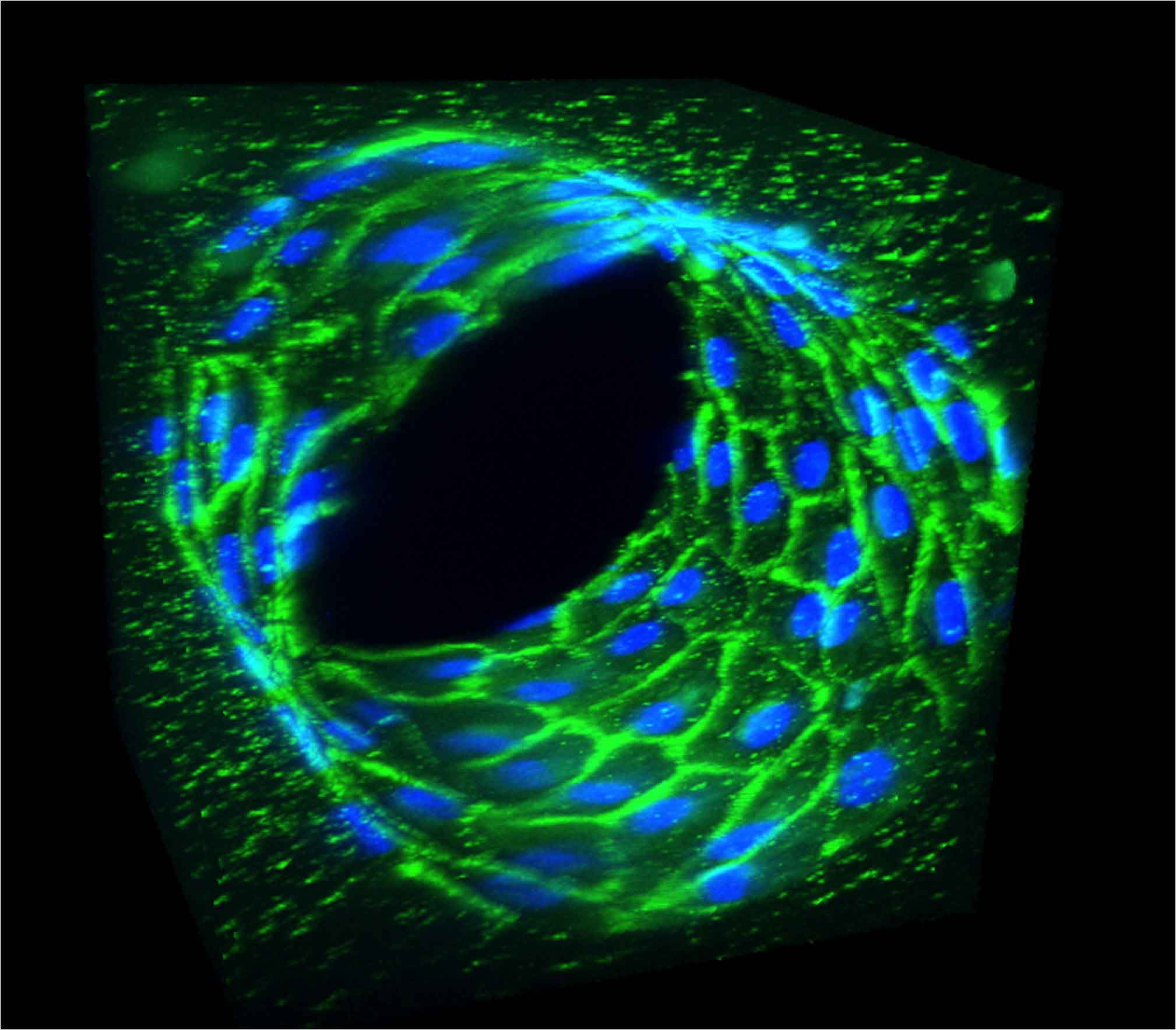
This 3D projection of a confocal microscope image (z-stack) shows human umbilical-vein endothelial cells forming a functional blood vessel stained for PECAM-1 (green) and nuclei (blue) (credit: Wong/Searson Lab)
Wong also created a video (above) of single cancer cells prying and pushing their way through the wall of an artificial vessel lined with human endothelial cells, the same kind that line human blood vessels.
By entering the bloodstream through this process, called “intravasion,” cancer cells are able to hitch a ride to other parts of the body and begin to form deadly new tumors.
The breast cancer cells, inserted individually and in clusters in the tissue near the vessel, are labeled with fluorescent tags, enabling their behavior to be seen, tracked and recorded via a microscopic viewing system.
Wong’s doctoral advisor, Peter Searson, the Joseph R. and Lynn C. Reynolds Professor of Materials Science and Engineering and director of the INBT, said Wong took on this challenging project nearly five years ago—and ultimately produced impressive results.
“In the past, it’s been virtually impossible to see the steps involved in this process with this level of clarity. We’ve taken a significant leap forward.”
Testing various anticancer strategies
This improved view should give cancer researchers a much clearer look at the complex physical and biochemical interplay that takes place when cells leave a tumor, move through the surrounding tissue and approach a blood vessel. For example, the new lab device enabled the inventors to see detailed images of a cancer cell as it found a weak spot in the vessel wall, exerted pressure on it and squeezed through far enough so that the force of the passing current swept it into the circulating fluid.
“This device allows us to look at the major steps of metastasis as well as to test different treatment strategies at a relatively fast pace,” Wong said. “If we can find a way to stop one of these steps in the metastatic cascade, we may be able to find a new strategy to slow down or even stop the spread of cancer.”
Next, the researchers plan to use the device to try out various cancer-fighting drugs within this device to get a better look at how the medications perform and how they might be improved. A provisional patent has been obtained through the Johns Hopkins Technology Transfer office.
INBT’s science writer, Mary Spiro, interviewed Wong for the NanoByte Podcast here.
Wong’s work has been supported by an INBT training grant. Development of the cancer research device was supported by the National Institutes of Health.
Abstract of Live-Cell Imaging of Invasion and Intravasation in an Artificial Microvessel Platform
Methods to visualize metastasis exist, but additional tools to better define the biologic and physical processes underlying invasion and intravasation are still needed. One difficulty in studying metastasis stems from the complexity of the interface between the tumor microenvironment and the vascular system. Here, we report the development of an investigational platform that positions tumor cells next to an artificial vessel embedded in an extracellular matrix. On this platform, we used live-cell fluorescence microscopy to analyze the complex interplay between metastatic cancer cells and a functional artificial microvessel that was lined with endothelial cells. The platform recapitulated known interactions, and its use demonstrated the capabilities for a systematic study of novel physical and biologic parameters involved in invasion and intravasation. In summary, our work offers an important new tool to advance knowledge about metastasis and candidate antimetastatic therapies. Cancer Res; 74(17); 4937–45. ©2014 AACR.