New ‘lab-on-a-chip’ could revolutionize early diagnosis of cancer
October 8, 2014
Illustration of a “lab of a chip” for detecting lung-cancer cells. The device is made of a widely used silicone rubber called polydimethylsiloxane and uses a technique called “on-chip immunoisolation.” (Credit: University of Kansas/KU News Service)
A new miniaturized biomedical “lab-on-a-chip” testing device for exosomes — molecular messengers between cells — promises faster, earlier, less-invasive diagnosis of cancer, according to its developers at the University of Kansas Medical Center and the University of Kansas Cancer Center.
“A lab-on-a-chip shrinks the pipettes, test tubes and analysis instruments of a modern chemistry lab onto a microchip-sized wafer,” explained Yong Zeng, assistant professor of chemistry at the University of Kansas.
Zeng and his fellow researchers developed the lab-on-a-chip initially for early detection of lung cancer — the number-one cancer killer in the U.S.
Lung cancer is currently detected mostly with an invasive biopsy, after tumors are larger than 3 centimeters in diameter and even metastatic. Using the lab-on-a-chip, lung cancer could be detected much earlier, using only a small drop of a patient’s blood, according to Zeng.
How it works
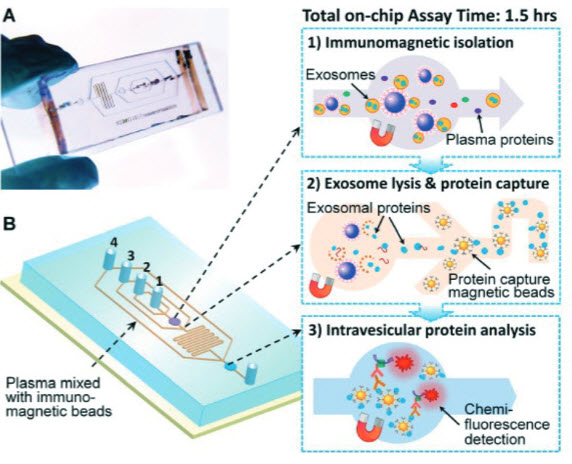
Integrated microfluidic exosome analysis directly from human
plasma. (A) Image of the prototype PDMS chip containing a cascading microchannel network for multi-stage exosome analysis. (B) Streamlined workflow for on-chip immunomagnetic isolation, chemical lysis, and intravesicular protein analysis of circulating exosomes. #1-4 indicates the inlet for exosome capture beads, washing/lysis buffer, protein capture beads, and ELISA reagents, respectively. (Credit: Mei He et al./Royal Society of Chemistry)
The prototype lab-on-a-chip is made of a widely used silicone rubber called polydimethylsiloxane and uses a technique called “on-chip immunoisolation.”
“We used magnetic beads of 3 micrometers in diameter to pull down the exosomes in plasma samples,” Zeng said. “To avoid other interfering species present in plasma, the bead surface was chemically modified with an antibody that recognizes and binds with a specific target protein — for example, a protein receptor — present on the exosome membrane. The plasma containing magnetic beads then flows through the microchannels on the diagnostic chip in which the beads can be readily collected using a magnet to extract circulating exosomes from the plasma.”
“Our technique provides a general platform to detecting tumor-derived exosomes for cancer diagnosis,” he said. “We’ve also tested for ovarian cancer in this work. In theory, it should be applicable to other types of cancer. Our long-term goal is to translate this technology into clinical investigation of the pathological implication of exosomes in tumor development. Such knowledge would help develop better predictive biomarkers and more efficient targeted therapy to improve the clinical outcome.”
The research by Zeng and his KU colleagues was described in a paper published in the Royal Society of Chemistry journal, and has been awarded a $640,000 grant from the National Cancer Institute at the National Institutes of Health, intended to further develop the lab-on-a-chip technology.
Abstract of Integrated immunoisolation and protein analysis of circulating exosomes using microfluidic technology
Developing blood-based tests is appealing for non-invasive disease diagnosis, especially when biopsy is difficult, costly, and sometimes not even an option. Tumor-derived exosomes have attracted increasing interest in non-invasive cancer diagnosis and monitoring of treatment response. However, the biology and clinical value of exosomes remains largely unknown due in part to current technical challenges in rapid isolation, molecular classification and comprehensive analysis of exosomes. Here we developed a new microfluidic approach to streamline and expedite the exosome analysis pipeline by integrating specific immunoisolation and targeted protein analysis of circulating exosomes. Compared to the conventional methods, our approach enables selective subpopulation isolation and quantitative detection of surface and intravesicular biomarkers directly from a minimally invasive amount of plasma samples (30 μL) within ~100 min with markedly improved detection sensitivity. Using this device, we demonstrated phenotyping of exosome subpopulations by targeting a panel of common exosomal and tumor-specific markers and multiparameter analyses of intravesicular biomarkers in the selected subpopulation. We were able to assess the total expression and phosphorylation levels of IGF-1R in non-small-cell lung cancer patients by probing plasma exosomes as a non-invasive alternative to conventional tissue biopsy. We foresee that the microfluidic exosome analysis platform will form the basis for critically needed infrastructures for advancing the biology and clinical utilization of exosomes.