A hydrogel that destroys superbugs and drug-resistant biofilms
January 28, 2013

Biofilm after treatment (credit: IBN)
The first-ever antimicrobial hydrogel that can break apart biofilms and destroy multidrug-resistant superbugs upon contact has been developed by researchers from the Institute of Bioengineering and Nanotechnology (IBN) and IBM Research.
Tests have demonstrated the effectiveness of this novel synthetic material in eliminating various types of bacteria and fungi that are leading causes of microbial infections, and preventing them from developing antibiotic resistance.
This discovery could be used in wound healing, medical device and contact lens coating, skin infection treatment, and dental fillings.
The synthetic gel is biodegradable, biocompatible and cost-effective. With over 90% water content, the hydrogel is highly flexible and easy to adapt for different uses. This gel can target the bacteria and fungi behind seven of the most common hospital-acquired infections such as MRSA (methicillin-resistant Staphylococcus aureus), VRE (vancomycin-resistant enterococcus), multidrug-resistant Acinetobacter baumannii and Klebsiella pneumoniae, E. coli, Candida albicans and Cryptococcus neoformans fungi.
This new gel is comprised of the novel polymer material jointly developed by IBN and IBM Research in 2010. When mixed with water and heated to body temperature, the polymers form spontaneously into a moldable gel, due to the self-associative interactions between the polymer molecules. This allows the hydrogel to target multidrug-resistant biofilms at various parts of the body and surfaces without being flushed away. Once the antimicrobial function is activated and performed, the biodegradable gel can be naturally eliminated by the body.
Using the new polymer material as a basic building block, IBN can now provide a comprehensive antimicrobial solution to combat drug-resistant bacteria and fungi for a range of medical and consumer products.
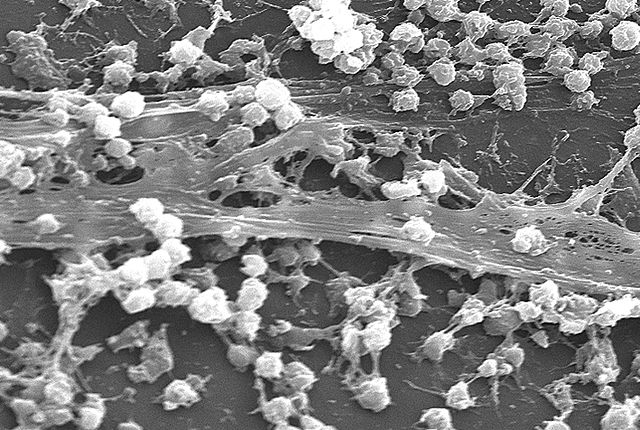
Staphylococcus aureus biofilm (credit: Wikimedia Commons)
Most microbial infections biofilm-related
More than 80% of all human microbial infections are related to biofilm. This is particularly challenging for infections associated with the use of medical equipment and devices. Biofilms are microbial cells that can easily colonize on almost any tissue or surface. They contribute significantly to hospital-acquired infections, which are among the top five leading causes of death in the U.S. and account for US$11 billion in healthcare spending each year.
In Singapore, antimicrobial drug resistance is a major healthcare problem because of the extensive use of antibiotics and medical equipment such as intravascular catheters and orthopedic implants in patients. Once in the body, these instruments become potential breeding grounds for bacterial growth. This provides a continuous source of contamination, which could result in prolonged hospitalization, higher medical costs, and greater risk of death.
Research has shown that patients in Singapore with microbial infections were 10.2 times more likely to die during their hospitalization, had 4.6 times longer hospitalization, and incurred 4 times higher hospitalization cost compared to patients with no infections.The emergence of new strains of superbugs and shortage of new drugs has exacerbated the need for an effective antimicrobial solution. Traditional household antiseptics and disinfectants are also proving to be ineffective in eliminating drug-resistant germs.
This research is funded by the Institute of Bioengineering and Nanotechnology. ETPL, the technology transfer arm of the Agency for Science, Technology and Research, funded the skin biocompatibility testing of the antimicrobial hydrogel for its commercial development for consumer care.