Virus brain-mapping technique uncovers circuits involved in Parkinson’s disease and Huntington’s disease
June 28, 2013
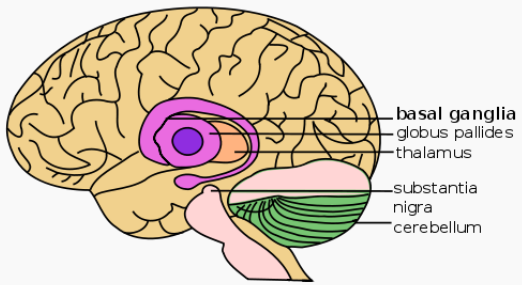
Basal ganglia (credit: Wikimedia Commons)
Gladstone Institutes and Salk Institute researchers have assembled brain-wide maps of neurons that connect with the basal ganglia, a region of the brain involved in movement and decision-making.
Developing a better understanding of this region is important as it could inform research into disorders causing basal ganglia dysfunction, including Parkinson’s disease and Huntington’s disease.
Team leaders Gladstone Investigator Anatol Kreitzer, PhD, and Salk Investigator Edward Callaway, PhD combined mouse models with a sophisticated tracing technique known as the monosynaptic rabies virus system.
“Taming and harnessing the rabies virus — as pioneered by Callaway — is ingenious in the exquisite precision that it offers compared with previous methods, which were messier with a much lower resolution,” explained Kreitzer, who is also an associate professor of neurology and physiology at the University of California, San Francisco, with which Gladstone is affiliated.
“We took the approach one step further by activating the tracer genetically, which ensures that it is only turned on in specific neurons in the basal ganglia. This is a huge leap forward technologically, as we can be sure that we’re following only the networks that connect to particular kinds of cells in the basal ganglia.”
At Gladstone, Kreitzer focuses his research on the role of the basal ganglia in Parkinson’s and other neurological disorders. Last year, he and his team published research that revealed clues to the relationship between two types of neurons found in the region — and how they guide both movement and decision-making.
These two types, called direct-pathway medium spiny neurons (dMSNs) and indirect-pathway medium spiny neurons (iMSNs), act as opposing forces. dMSNs initiate movement, like the gas pedal, and iMSNs inhibit movement, like the brake.
The latest research from the Kreitzer lab further found that these two types are also involved in decision-making behavior, and that a dysfunction of dMSNs or iMSNs is associated with addictive or depressive behaviors, respectively. These findings were important because they provided a link between the physical neuronal degeneration seen in movement disorders, such as Parkinson’s, and some of the disease’s behavioral aspects. But this study still left many questions unanswered, such as how other brain regions influenced the function of these two neuron types.
Tracing brain pathways
The monosynaptic rabies virus system uses a modified version of the rabies virus to “infect” a brain region, which in turn targets neurons that are connected to it. When the system was applied in genetic mouse models, the team could see specifically how sensory, motor, and reward structures in the brain connected to MSNs in the basal ganglia. And what they found was surprising.
“We noticed that some regions showed a preference for transmitting to dMSNs versus iMSNs, and vice versa,” said Kreitzer. “For example, neurons residing in the brain’s motor cortex tended to favor iMSNs, while neurons in the sensory and limbic systems preferred dMSNs. This fine-scale organization, which would have been virtually impossible to observe using traditional techniques, allows us to predict the distinct roles of these two neuronal types.”
“These initial results should be treated as a resource not only for decoding how this network guides the vast array of very distinct brain functions, but also how dysfunctions in different parts of this network can lead to different neurological conditions,” said Callaway. “If we can use the rabies virus system to pinpoint distinct network disruptions in distinct types of disease, we could significantly improve our understanding of these diseases’ underlying molecular mechanisms — and get even closer to developing solutions for them.”
This research was supported by the Gatsby Charitable Foundation and the National Institutes of Health.