New candidate drug stops cancer cells, regenerates nerve cells
June 28, 2012
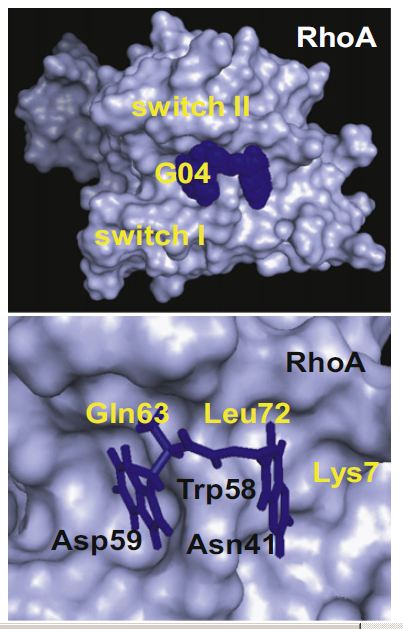
A simulated docking model of G04 on RhoA surface. (Upper) Top view of the binding pocket of RhoA bound to G04. (Lower) Top view of the predicted structural contacts of G04 in the binding pocket around Trp58 of RhoA. (Credit: Xun Shang et al./Chemistry & Biology)
A small-molecule-inhibiting drug called Rhosin that in early laboratory cell tests stopped breast cancer cells from spreading and promotes the growth of early nerve cells called neurites has been developed by researchers at Cincinnati Children’s Hospital Medical Center
The inhibitor drug precisely targets a single component of a cell signaling protein complex called Rho GTPases that regulates cell movement and growth throughout the body. Miscues in Rho GTPase processes are widely implicated in human diseases, including various cancers and neurologic disorders.
“Although still years from clinical development, in principle Rhosin could be useful in therapy for many kinds of cancer or possibly neuron and spinal cord regeneration,” said Yi Zheng, PhD, lead investigator and director of Experimental Hematology and Cancer Biology at Cincinnati Children’s. “
We’ve performed in-silica (computerized) rational drug design, pharmacological characterization and cell tests in the laboratory, and we are now starting to work with mouse models.”
Because the role of Rho GTPases in cellular processes and cancer formation is well established, researchers have spent years trying to identify safe and effective therapeutic targets for specific parts of the protein complex.
In particular, scientists have focused on the center protein in the complex called RhoA, which is essential for the signaling function of the complex. In breast cancer for example, increased RhoA activity makes the cancer cells more invasive and causes them to spread, while a deficiency of RhoA suppresses cancer growth and progression.
Despite this knowledge, past efforts to develop an effective small-molecule inhibitor for RhoA have failed, explained Zheng, who has studied Rho GTPases for over two decades. Most roadblocks stem from a lack of specificity in how researchers have been able to target RhoA, a resulting lack of efficiency in affecting molecular processes, problems with toxicity, and the inability to find a workable drug design.
For the current study, Zheng and his colleagues used high-throughput computerized molecular screening and computerized drug design to reveal a druggable target site. This also provided a preliminary virtual simulation on the potential effectiveness of candidate drugs.
A key challenge to binding a small-molecule inhibitor to RhoA is the protein’s globular structure and lack of surface pocket areas suitable for easy binding, Zheng said. The unique chemical structure of the lead compound identified by researchers, Rhosin, allows it to effectively bind to two shallow surface grooves on RhoA. This enables the candidate drug to take root and begin affecting cells. The two-legged configuration of Rosin also describes a useful drug design strategy for more effectively targeting difficult molecular sites like RhoA.
The researchers also wanted to make sure Rhosin effectively blocked what are known as guanine nucleotide exchange factors (GEFs). Guanine nucleotide is a critical energy source and signaling component of cells. Activation of GEFs is required to set off the regulatory signaling of GTPases (GTP stands for guanosine triphosphate).
Lab tests
In tests on a human breast cancer cells, Rhosin inhibited cell growth and the formation of mammary spheres in a dose dependent manner, acting specifically on RhoA molecular targets without disrupting other critical cellular processes. Rhosin does not affect non-cancerous breast cells. This, along with other tests the scientists performed, indicated Rhosin’s effectiveness in targeting RhoA-mediated breast cancer proliferation, according to the researchers.
Researchers also treated an extensively tested line of neuronal cells with Rhosin, along with nerve growth factor, a protein that is important to the growth and survival of neurons. Rhosin worked with nerve growth factor in a dose-dependent way to promote the proliferation of branching neurites from the neuronal cells.
Also collaborating on the study were NanoTemper Technologies in Munich, Germany and the Drug Discovery Center at the University of Cincinnati. Funding for the study came from National Institutes of Health.