Study suggests probiotics could prevent obesity and insulin resistance
July 25, 2014
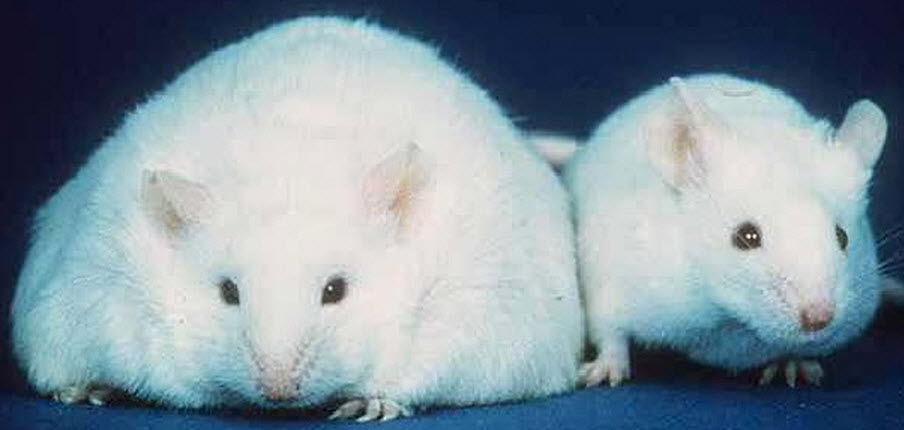
Obese vs. lean mouse (credit: Wikimedia Commons)
Vanderbilt University researchers have discovered that engineered probiotic bacteria (“friendly” bacteria like those in yogurt) in the gut produce a therapeutic compound that inhibits weight gain, insulin resistance, and other adverse effects of a high-fat diet in mice.
“Of course it’s hard to speculate from mouse to human,” said senior investigator Sean Davies, Ph.D., assistant professor of Pharmacology. “But essentially, we’ve prevented most of the negative consequences of obesity in mice, even though they’re eating a high-fat diet.”
The findings published in the August issue of the Journal of Clinical Investigation (open access) suggest that it may be possible to manipulate the bacterial residents of the gut — the gut microbiota — to treat obesity and other chronic diseases.
Davies has a long-standing interest in using probiotic bacteria to deliver drugs to the gut in a sustained manner, in order to eliminate the daily drug regimens associated with chronic diseases. In 2007, he received a National Institutes of Health Director’s New Innovator Award to develop and test the idea.
Manipulating gut bacteria to promote health
Other studies have demonstrated that the natural gut microbiota plays a role in obesity, diabetes and cardiovascular disease. “The types of bacteria you have in your gut influence your risk for chronic diseases,” Davies said. “We wondered if we could manipulate the gut microbiota in a way that would promote health.”
To start, the team needed a safe bacterial strain that colonizes the human gut. They selected E. coli Nissle 1917, which has been used as a probiotic treatment for diarrhea since its discovery nearly 100 years ago.
They genetically modified the E. coli Nissle strain to produce a lipid compound called N-acyl phosphatidylethanolamine (NAPE)*, which is normally synthesized in the small intestine in response to feeding. NAPE is rapidly converted to NAE, a compound that reduces both food intake and weight gain. Some evidence suggests that NAPE production may be reduced in individuals eating a high-fat diet.
“NAPE seemed like a great compound to try — since it’s something that the host normally produces,” Davies said.
The investigators added the NAPE-producing bacteria to the drinking water of mice eating a high-fat diet for eight weeks. Mice that received the modified bacteria had dramatically lower food intake, body fat, insulin resistance and fatty liver compared to mice receiving control bacteria.
They found that these protective effects persisted for at least four weeks after the NAPE-producing bacteria were removed from the drinking water. And even 12 weeks after the modified bacteria were removed, the treated mice still had much lower body weight and body fat compared to the control mice. Active bacteria no longer persisted after about six weeks.
“We still haven’t achieved our ultimate goal, which would be to do one treatment and then never have to administer the bacteria again,” Davies said. “Six weeks is pretty long to have active bacteria, and the animals are still less obese 12 weeks out. “This paper provides a proof of concept,” he said. “Clearly, we can get enough bacteria to persist in the gut and have a sustained effect. We would like for that effect to last longer.”
Davies noted that the researchers also observed effects of the compounds in the liver, suggesting that it may be possible to use modified bacteria to deliver therapeutics beyond the gut.
The investigators are currently working on strategies to address regulatory issues related to containing the bacteria, for example by knocking out genes required for the bacteria to live outside the treated host.
So when can we expect a weight-loss pill?
“It is likely to be at least several years, as we need to further engineer the bacteria with additional safety mechanisms in order to gain approval from the FDA for clinical trials, and then these trials would need to be conducted,” Davies explained to KurzweilAI in an email interview. “For human clinical trials, additional safety mechanisms will have to be engineered into the bacteria.”
Davies noted that currently, there are two standard treatments for obesity: diet/exercise and bariatric surgery. “As many people have experienced, losing weight using diet/exercise is often highly effective in the short-term, but generally difficult to maintain for the long-term. Bariatric surgery is quite helpful for those that are morbidly obese, but the initial risk of the surgery is significant.
“Our hope is that by engineering the gut microbiota to produce NAPE, we can create sustained weight loss for very long periods of time, with only relatively infrequent booster doses of bacteria.
“While it might be possible to create the same effect as with our bacteria simply by injection of the NAPE everyday, in general, long-term compliance with medications that have to be taken every day is quite poor. The key point we are trying to achieve, and that our paper shows proof-of-concept for, is creating sustained drug delivery by engineering the gut microbiota to make the therapeutic compound.”
This research was supported by the New Innovator Award and by other grants from the National Institutes of Health.
* Curiously, NAPES are also important intermediaries in the biosynthesis of endocannabinoids, as noted in this Wikipedia post. “The endocannabinoid system is a group of neuromodulatory lipids and their receptors in the brain that are involved in a variety of physiological processes including appetite, pain-sensation, mood, and memory; it mediates the psychoactive effects of cannabis [the active ingredient of marijuana].” Could this also explain “the munchies”?
Abstract of Journal of Clinical Investigation paper
Metabolic disorders, including obesity, diabetes, and cardiovascular disease, are widespread in Westernized nations. Gut microbiota composition is a contributing factor to the susceptibility of an individual to the development of these disorders; therefore, altering a person’s microbiota may ameliorate disease. One potential microbiome-altering strategy is the incorporation of modified bacteria that express therapeutic factors into the gut microbiota. For example, N-acylphosphatidylethanolamines (NAPEs) are precursors to the N-acylethanolamide (NAE) family of lipids, which are synthesized in the small intestine in response to feeding and reduce food intake and obesity. Here, we demonstrated that administration of engineered NAPE-expressing E. coli Nissle 1917 bacteria in drinking water for 8 weeks reduced the levels of obesity in mice fed a high-fat diet. Mice that received modified bacteria had dramatically lower food intake, adiposity, insulin resistance, and hepatosteatosis compared with mice receiving standard water or control bacteria. The protective effects conferred by NAPE-expressing bacteria persisted for at least 4 weeks after their removal from the drinking water. Moreover, administration of NAPE-expressing bacteria to TallyHo mice, a polygenic mouse model of obesity, inhibited weight gain. Our results demonstrate that incorporation of appropriately modified bacteria into the gut microbiota has potential as an effective strategy to inhibit the development of metabolic disorders.