Tissue scaffold technology could help rebuild large organs
June 18, 2015
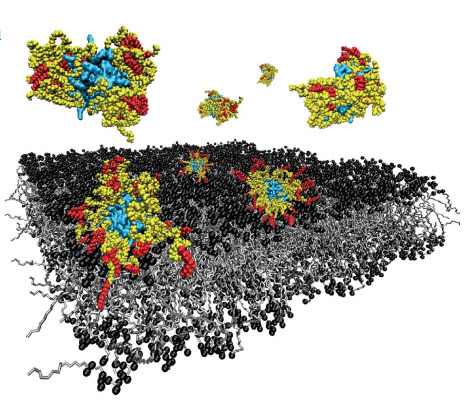
A novel polymer–surfactant complex of oxygen-carrying protein myoglobin is delivered to the cytoplasmic membrane of stem cells, which are then used to engineer cartilage constructs with significantly enhanced oxygen distribution to the center of the tissue (credit: James P.K. Armstrong et al./Nature Communications)
Researchers at the Universities of Bristol and Liverpool have developed a new tissue scaffold (support structure) technology that could one day make it possible to engineer large organs.
Currently, tissue engineering has been limited to growing small pieces of tissue, because larger dimensions reduce the oxygen supply to the cells in the center of the tissue.
The team of researchers, led by Adam Perriman from the University of Bristol and Professor Anthony Hollander from the University of Liverpool, synthesized a new class of artificial membrane binding proteins that can be attached to stem cells.
By attaching an oxygen-carrying protein, myoglobin, to the stem cells before they are used to engineer cartilage, they ensure that each cell has its own oxygen reservoir that it can access when the oxygen in the scaffold drops to dangerously low levels.
The team’s open-access findings, published June 18 in Nature Communications, could expand the possibilities in tissue engineering, including other tissue such as cardiac muscle or bone.
“Creating larger pieces of cartilage gives us a possible way of repairing some of the worst damage to human joint tissue, such as the debilitating changes seen in hip or knee osteoarthritis or the severe injuries caused by major trauma, for example in road traffic accidents or war injuries,” said Hollander.
Hollander’s pioneering work includes the development of a method of creating cartilage cells from stem cells, which helped to make possible the first successful transplant of a tissue-engineered trachea, using the patient’s own stem cells.
Abstract of Artificial membrane-binding proteins stimulate oxygenation of stem cells during engineering of large cartilage tissue
Restricted oxygen diffusion can result in central cell necrosis in engineered tissue, a problem that is exacerbated when engineering large tissue constructs for clinical application. Here we show that pre-treating human mesenchymal stem cells (hMSCs) with synthetic membrane-active myoglobin-polymer–surfactant complexes can provide a reservoir of oxygen capable of alleviating necrosis at the centre of hyaline cartilage. This is achieved through the development of a new cell functionalization methodology based on polymer–surfactant conjugation, which allows the delivery of functional proteins to the hMSC membrane. This new approach circumvents the need for cell surface engineering using protein chimerization or genetic transfection, and we demonstrate that the surface-modified hMSCs retain their ability to proliferate and to undergo multilineage differentiation. The functionalization technology is facile, versatile and non-disruptive, and in addition to tissue oxygenation, it should have far-reaching application in a host of tissue engineering and cell-based therapies.